Connect With Us
Blog

Gout
Gout is a form of arthritis that is caused by a buildup of uric acid crystals in the joints. This considered to be one of the most frequently recorded medical illnesses throughout history. Gout occurrences in the US have risen within the past twenty years and the condition now affects 8.3 million people which is 4% of all Americans. Researchers have found that gout affects men more than women and African-American men more than white men.
Symptoms of gout are warmth, swelling, discoloration, and tenderness in the affected joint area. The small joint on the big toe is the most common place for a gout attack to occur.
People who are obese, gain weight excessively, drink alcohol heavily, have high blood pressure, or have abnormal kidney function are more likely to develop gout. Furthermore, certain drugs and diseases are likely to increase levels of uric acid in the joints which eventually leads to gout. You are also more likely to develop gout if you eat a lot of meat and fish.
Many who experience gout attacks will experience repeated attacks over the years. Some people who have gout symptoms, may never have them again, but others may experience them several times a year. If you have gout symptoms throughout the year, you may have recurrent gout. Those who have gout should also be careful about their urate crystals collecting in their urinary tract, because this may lead to kidney stones.
Diagnosis for gout is done by checking the level of uric acid in the joints and blood. Your podiatrist may also prescribe medicine to reduce uric acid buildup in the blood, which will help prevent any gout attacks.
To treat gout, your podiatrist may also prescribe you Anti-inflammatory medication (NSAIDs) which will relieve the pain and swelling of a gout episode and it can also shorten a gout attack. Maintaining a healthy diet is also a proven method to prevent gout attacks.
Understanding Your Child’s Heel Pain
 Your child may experience heel pain during a growth spurt. This condition is commonly known as Sever’s disease. Since the heel grows faster than the rest of the leg, the tendons experience extra strain. Symptoms of Sever’s disease include pain in one or both of the heels, tenderness that increases during exercise, and trouble walking. Oftentimes, the best treatment is rest. The condition does not cause long-term issues and should subside after a few months. However, sometimes doctors will recommend that a child takes NSAIDs such as ibuprofen, performs stretching routines, and wears supportive shoes. Be especially cognizant for Sever’s disease if your child plays a sport that includes running or jumping on hard surfaces. If your child is experiencing heel pain, be sure to contact a podiatrist.
Your child may experience heel pain during a growth spurt. This condition is commonly known as Sever’s disease. Since the heel grows faster than the rest of the leg, the tendons experience extra strain. Symptoms of Sever’s disease include pain in one or both of the heels, tenderness that increases during exercise, and trouble walking. Oftentimes, the best treatment is rest. The condition does not cause long-term issues and should subside after a few months. However, sometimes doctors will recommend that a child takes NSAIDs such as ibuprofen, performs stretching routines, and wears supportive shoes. Be especially cognizant for Sever’s disease if your child plays a sport that includes running or jumping on hard surfaces. If your child is experiencing heel pain, be sure to contact a podiatrist.
Sever's disease often occurs in children and teens. If your child is experiencing foot or ankle pain, see one of our podiatrists from Pennsylvania Foot & Ankle. Our doctors can treat your child’s foot and ankle needs.
Sever’s Disease
Sever’s disease is also known as calcaneal apophysitis, which is a medical condition that causes heel pain I none or both feet. The disease is known to affect children between the ages of 8 and 14.
Sever’s disease occurs when part of the child’s heel known as the growth plate (calcaneal epiphysis) is attached to the Achilles tendon. This area can suffer injury when the muscles and tendons of the growing foot do not keep pace with bone growth. Therefore, the constant pain which one experiences at the back of the heel will make the child unable to put any weight on the heel. The child is then forced to walk on their toes.
Symptoms
Acute pain – Pain associated with Sever’s disease is usually felt in the heel when the child engages in physical activity such as walking, jumping and or running.
Highly active – Children who are very active are among the most susceptible in experiencing Sever’s disease, because of the stress and tension placed on their feet.
If you have any questions, please feel free to contact one of our offices located in Bensalem, Philadelphia, Northeast Philadelphia, Yardley, PA, and Hamilton, NJ . We offer the newest diagnostic and treatment technologies for all your foot care needs.
Sever's Disease
Sever’s disease, also known as calcaneal apophysitis is a common bone disorder that occurs during childhood. The disease is defined as an inflammation of the growth plate in the heel. When a child has a growth spurt, his heel bone grows faster than the muscles, tendons, and ligaments in his leg. This disease is a result of overuse. The people who are most likely to be affected by this disease are children who are in a growth spurt, especially boys who are from the ages of 5 to 13 years old. 60% of children with Sever’s disease have both heels involved.
Symptoms of this disease are heel pain that intensifies during running and jumping activities. The pain is typically localized to the posterior part of the heel. Symptoms may be severe, and they can easily interfere with daily activities. Children who play soccer, baseball, and basketball are more likely to develop Sever’s disease.
Your doctor will diagnose your child based on his or her symptoms, x-rays are generally not helpful in diagnosing this disease. Your doctor may examine both heels and ask your child questions about his or her activity level in sports. Your doctor may then use the squeeze test on your child’s heel to see if there is any pain. Nevertheless, some doctors might still use x-rays to rule out any other issues such as fractures, infections, and tumors.
Sever’s disease can be prevented by maintaining good flexibility while your child is growing. Another prevention method is to wear good-quality shoes that have firm support and a shock-absorbent sole. Sever’s disease can be treated by ceasing any activity that causes heel pain. You should apply ice to the injured heel for 20 minutes 3 times a day. Additionally, orthotics should be used for children who have high arches, flat feet, or bowed legs.
If you suspect your child has Sever’s disease, you should make an appointment with your podiatrist to have his or her foot examined. Your doctor may recommend nonsteroidal anti-inflammatory drugs (NSAIDs), such as ibuprofen or naproxen to relieve pain. In more severe cases, your child may need a cast to rest his or her heel. Fortunately, Sever’s disease does not cause long-term foot problems. After treatment, your child should start to feel better within two weeks to two months.
Edema and Pregnancy
Many pregnant women notice their feet have become swollen. This is caused by the pressure that is put on the lower limbs, which is often the result of a growing fetus. The medical term for excessive swelling is referred to as edema, and is a common ailment in a large percentage of pregnant women. It is beneficial to wear shoes that are comfortable, and elevating the legs frequently during the day may bring mild relief. Additionally, the feet may swell as a result of high blood pressure. Research has shown if one foot becomes swollen, it may be indicative of an existing medical condition. If you would like additional information about how pregnancy affects the feet, it is suggested that you schedule a consultation with a podiatrist.
Pregnant women with swollen feet can be treated with a variety of different methods that are readily available. For more information about other cures for swollen feet during pregnancy, consult with one of our podiatrists from Pennsylvania Foot & Ankle. Our doctors will attend to all of your foot and ankle needs.
What Foot Problems Can Arise During Pregnancy?
One problem that can occur is overpronation, which occurs when the arch of the foot flattens and tends to roll inward. This can cause pain and discomfort in your heels while you’re walking or even just standing up, trying to support your baby.
Another problem is edema, or swelling in the extremities. This often affects the feet during pregnancy but tends to occur in the later stages.
How Can I Keep My Feet Healthy During Pregnancy?
- Wearing orthotics can provide extra support for the feet and help distribute weight evenly
- Minimize the amount of time spent walking barefoot
- Wear shoes with good arch support
- Wear shoes that allow for good circulation to the feet
- Elevate feet if you experience swelling
- Massage your feet
- Get regular, light exercise, such as walking, to promote blood circulation to the feet
If you have any questions, please feel free to contact one of our offices located in Bensalem, Philadelphia, Northeast Philadelphia, Yardley, PA, and Hamilton, NJ . We offer the newest diagnostic and treatment technologies for all your foot care needs.
Foot Care for Pregnant Women
The natural weight that pregnant women gain causes their center of gravity to be completely altered. This causes them to have a new weight-bearing stance which adds pressure to the knees and feet. As a result, pregnant women often experience severe foot pain. The two most common foot issues experienced by women in their pregnancies are edema and over-pronation. It is important for all pregnant women to learn more about how to take care of their feet so they are more comfortable during their pregnancy.
Over-pronation, which is commonly referred to as flat feet, is caused when a person’s arch flattens out upon weight bearing. This causes the person’s feet to roll inward while walking. Pregnant women often experience this due to the sudden weight they gain.
Edema, also referred as swelling in the feet, typically occurs in the later part of the pregnancy. It is the result of the extra blood accumulated in the pregnant woman’s body. The enlarged uterus puts more pressure on the blood vessels in the pelvis which causes leg circulation to slow down. This causes blood to pool in the lower extremities.
Fortunately, there are ways to treat both edema and over-pronation. Edema can be treated by elevating the foot as often as possible. Wearing proper fitting footwear will also be helpful for those with edema. A treatment method for over-pronation could be orthotics. Orthotic inserts should be designed with appropriate arch support and medial rear foot for your foot.
It is best for pregnant women to buy new shoes during the day, because this is the time where swelling is at its peak. Pregnant women also shouldn’t rush when buying shoes. It is always advised that you make sure your shoes fit properly but this is especially important during pregnancy.
If you are a pregnant woman, you should consult with a podiatrist in order to make sure your feet are healthy throughout the entirety of your pregnancy.
Arthritis Can Cause Pain in the Feet and Ankles
What Can Help Heel Spur Pain?
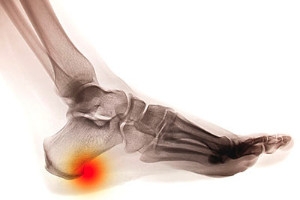
 A heel spur is a bony growth that forms on the heel of the foot. It consists of a calcium deposit which forms under the heel bone. This condition often produces severe pain and discomfort, and may become worse while putting pressure on the heel. Many patients find mild relief by wearing shoe inserts, as this may be beneficial in reducing impact on the heel. Additionally, it can help to wear shoes that have excess cushioning in the heel area, because this can aid in minimizing inflammation. A proper diagnosis is generally achieved by performing an X-ray of the foot, which can determine the size and location of the heel spur. If you have developed a heel spur, it is advised that you speak to a podiatrist so proper treatment can begin.
A heel spur is a bony growth that forms on the heel of the foot. It consists of a calcium deposit which forms under the heel bone. This condition often produces severe pain and discomfort, and may become worse while putting pressure on the heel. Many patients find mild relief by wearing shoe inserts, as this may be beneficial in reducing impact on the heel. Additionally, it can help to wear shoes that have excess cushioning in the heel area, because this can aid in minimizing inflammation. A proper diagnosis is generally achieved by performing an X-ray of the foot, which can determine the size and location of the heel spur. If you have developed a heel spur, it is advised that you speak to a podiatrist so proper treatment can begin.
Heel spurs can be incredibly painful and sometimes may make you unable to participate in physical activities. To get medical care for your heel spurs, contact one of our podiatrists from Pennsylvania Foot & Ankle. Our doctors will do everything possible to treat your condition.
Heels Spurs
Heel spurs are formed by calcium deposits on the back of the foot where the heel is. This can also be caused by small fragments of bone breaking off one section of the foot, attaching onto the back of the foot. Heel spurs can also be bone growth on the back of the foot and may grow in the direction of the arch of the foot.
Older individuals usually suffer from heel spurs and pain sometimes intensifies with age. One of the main condition's spurs are related to is plantar fasciitis.
Pain
The pain associated with spurs is often because of weight placed on the feet. When someone is walking, their entire weight is concentrated on the feet. Bone spurs then have the tendency to affect other bones and tissues around the foot. As the pain continues, the feet will become tender and sensitive over time.
Treatments
There are many ways to treat heel spurs. If one is suffering from heel spurs in conjunction with pain, there are several methods for healing. Medication, surgery, and herbal care are some options.
If you have any questions, please feel free to contact one of our offices located in Bensalem, Philadelphia, Northeast Philadelphia, Yardley, PA, and Hamilton, NJ . We offer the newest diagnostic and treatment technologies for all your foot care needs.
How to Treat Heel Spurs
Heel spurs are calcium deposits that cause bone protrusions on the heel bone. Heel spurs are usually associated with plantar fasciitis, which occurs when the plantar fasciitis in the foot becomes inflamed. Typically, heel spurs don’t cause any symptoms. However, they can produce chronic or intermittent heel pain. Those who have had the condition often describe the irritation as a stabbing pain.
There are risk factors that may make you more likely to develop heel spurs. People who have abnormal walking gaits, run and jog on hard surfaces, are obese, or wear poorly fitting shoes are more likely to develop heel spurs.
Fortunately, there are precautions you can take to avoid developing heel spurs. One of the best ways to do this is by wearing well-fitting shoes with shock-absorbent soles. Another preventative technique is to choose running shoes if you plan on running, and walking shoes if you plan on walking. Shoes are made for different activities and it is important to research a shoe before you purchase a pair.
The pain associated with heel spurs often decreases the more you walk. However, a recurrence of pain after an extended period of rest or walking is likely to occur with this condition. Those with severe heel spur pain may opt to go the surgical route for treatment. However, more than 90% of those with the condition get better without surgical treatment. If you have a heel spur and want to know if surgery is right for you, you should go to your podiatrist and he or she will be able to conduct a pre-surgical test or exam to determine if you are an optimal candidate for surgery.
Feet Tips For Diabetics
 Diabetics are at increased risk for foot complications, as many diabetics have reduced blood flow and damaged nerves. There are a few measures to take to protect your feet. First, examine your feet daily. If you cannot see your feet completely, use a mirror or have someone assist you. Look for cuts, discoloration, and sores. Make sure your toenails are cut and filed as well. Additionally, do not walk barefoot. You should assure that the lining on your shoes and socks are smooth before wearing them. Another step to remember is to avoid subjecting your feet to extreme temperatures. Check showers or bodies of water before entering. When possible, elevate your legs and wiggle your toes in order to help your circulation. Remembering these tips could prevent amputation, or even life-threatening complications. Diabetics should be going to a podiatrist twice a year for an exam, as well as speaking with a podiatrist when questions arise.
Diabetics are at increased risk for foot complications, as many diabetics have reduced blood flow and damaged nerves. There are a few measures to take to protect your feet. First, examine your feet daily. If you cannot see your feet completely, use a mirror or have someone assist you. Look for cuts, discoloration, and sores. Make sure your toenails are cut and filed as well. Additionally, do not walk barefoot. You should assure that the lining on your shoes and socks are smooth before wearing them. Another step to remember is to avoid subjecting your feet to extreme temperatures. Check showers or bodies of water before entering. When possible, elevate your legs and wiggle your toes in order to help your circulation. Remembering these tips could prevent amputation, or even life-threatening complications. Diabetics should be going to a podiatrist twice a year for an exam, as well as speaking with a podiatrist when questions arise.
Diabetic Limb Salvage
Diabetic limb salvage can be an effective way in preventing the need for limb amputation. If you have a foot ulcer and diabetes, consult with one of our podiatrists from Pennsylvania Foot & Ankle. Our doctors will assess your condition and provide you with quality foot and ankle treatment.
What Is Diabetic Limb Salvage?
Diabetic limb salvage is the attempt of saving a limb, such as the foot, that has an infected ulcer, from amputation. Podiatrists also try to make sure that there is enough function in the foot after the salvage that it is still usable. Those with diabetes experience poor blood circulation, which prevents proper healing of an ulcer. If the ulcer is left uncheck, it could become infected, which could result in the need for amputation.
Diabetes is the number one cause of non-traumatic amputations in the United States. Amputation has been found to lead to higher mortality rates. This translates into higher healthcare costs, and a reduced quality of life and mobility for amputees. Podiatrists have attempted to increase the prevalence of limb salvage in an attempt to solve these issues.
Diagnosis and Treatment
Limb salvage teams have grown in recent years that utilize a number of different treatments to save the infected limb. This includes podiatrists that specialize in wound care, rehabilitation, orthotics, and surgery. Through a combination of these methods, limb salvage has been found to be an effective treatment for infected limbs, and as an alternative to amputation. Podiatrists will first evaluate the potential for limb salvage and determine if the limb can be saved or must be amputated.
If you have any questions, please feel free to contact one of our offices located in Bensalem, Philadelphia, Northeast Philadelphia, Yardley, PA, and Hamilton, NJ . We offer the newest diagnostic and treatment technologies for all your foot care needs.
Blog Archives
- December 2025
- November 2025
- October 2025
- September 2025
- August 2025
- July 2025
- June 2025
- May 2025
- April 2025
- March 2025
- February 2025
- January 2025
- December 2024
- November 2024
- October 2024
- September 2024
- August 2024
- July 2024
- June 2024
- May 2024
- April 2024
- March 2024
- February 2024
- January 2024
- December 2023
- November 2023
- October 2023
- September 2023
- August 2023
- July 2023
- June 2023
- May 2023
- April 2023
- March 2023
- February 2023
- January 2023
- December 2022
- November 2022
- October 2022
- September 2022
- August 2022
- July 2022
- June 2022
- May 2022
- April 2022
- March 2022
- February 2022
- January 2022
- December 2021
- November 2021
- October 2021
- September 2021
- August 2021
- July 2021
- June 2021
- May 2021
- April 2021
- March 2021
- February 2021
- January 2021
- December 2020
- November 2020
- October 2020
- September 2020
- August 2020
- July 2020
- June 2020
- May 2020
- April 2020
- March 2020
- February 2020
- January 2020
- December 2019
- November 2019
- October 2019
- September 2019
- August 2019
- July 2019
- June 2019
- May 2019
- April 2019
- March 2019
- February 2019
- January 2019
- December 2018
- November 2018
- October 2018
- September 2018
- August 2018
- July 2018
- June 2018
- May 2018
- April 2018
- March 2018
- February 2018
- January 2018
- December 2017
- November 2017
- October 2017
- September 2017
- August 2017
- July 2017
- June 2017
- May 2017
- April 2017
- March 2017
- February 2017
- January 2017
- December 2016
- November 2016